My Understanding:
Statistics provide valuable insights into answering significant questions. However, all the content in this blog is my interpretation of data, shaped by my cultural background and a touch of logical reasoning. The connection between genetics and mental health raises a profound question: How much of our identity is inherited and how much is influenced by our experiences? Historically, people attempted to explain mental illness in simplistic terms. Some believed it was primarily biologically inherited through family bloodlines, while others attributed it to trauma, stress, environment, or upbringing. Today, research reveals that both perspectives are incomplete on their own. Mental health is not solely determined by genetics, but genetics can play a role in the starting point of our mental health journey.
Genes can increase the risk of certain mental health conditions. Disorders like schizophrenia, bipolar disorder, ADHD, autism, depression, anxiety, and PTSD all have some link to inherited biology. A person might be born with a nervous system that reacts more intensely to fear and other emotional stimuli. This doesn’t mean they’re broken; it simply means their mind and body process the world differently from others.
Genetics, while a significant factor, is not a predetermined fate. Having a family history of mental illness doesn’t guarantee that someone will develop the same condition. Genetics often creates vulnerability, but the environment plays a crucial role in determining whether that vulnerability manifests, remains dormant, or becomes manageable. Factors such as trauma, poverty, chronic stress and lack of support can elevate the risk of mental health issues. Conversely therapy, medication, a structured routine and a supportive community can shield individuals and enhance their overall well-being.
Post-traumatic stress disorder (PTSD) serves as a prime example of this intricate relationship. While genetics alone don’t cause PTSD, trauma is an essential precursor. Nevertheless, genetics can influence how the brain processes fear, memory, stress hormones and recovery after trauma. Two individuals who endure similar events may exhibit vastly different responses. This phenomenon underscores the profound individuality of minds, skin to fingerprints. These differences aren’t always indicative of strength or weakness. Instead, they may arise from a complex interplay of biology, environment, support, and timing, all converging into a unique pattern.
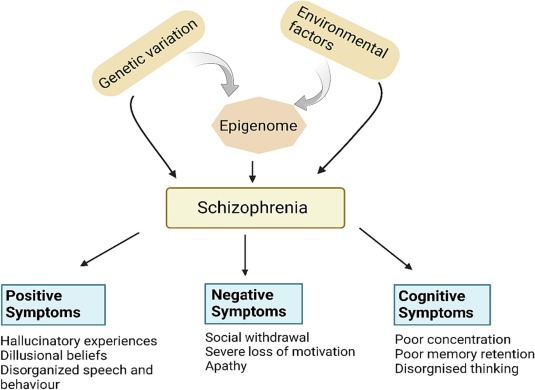
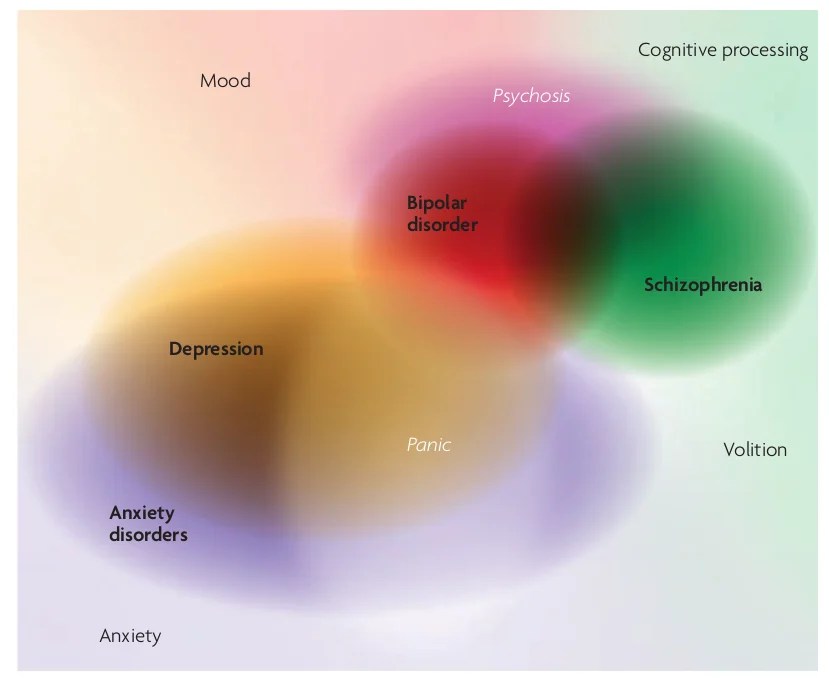
Many mental health conditions overlap because they don’t exist in distinct categories. The DSM (Diagnostic and Statistical Manual of Mental Disorders) primarily categorizes most disorders but has shifted towards incorporating spectrums and dimensional approaches for many conditions. Some share genetic risk factors, which explains why mental health conditions often run in families or appear together in the same person.
In the end, understanding genetics and mental health should foster compassion, not judgment. If mental illness has biological roots, it should not be dismissed as laziness or a lack of willpower. Furthermore, if the environment also plays a role, society cannot ignore trauma. This includes issues such as poverty, racism, violence, isolation, and limited access to care.
Genetics may provide the blueprint, but life molds the structure. No individual is solely defined by their DNA. Mental health is influenced by our experiences, the support we receive, and whether we have the opportunity to heal. Therefore, I leave you with this thought: if genetics offers the blueprint and life shapes the structure, how much responsibility do we, as a society, have to create environments where individuals are not merely surviving their biology, but healing beyond it?

"Let It Marinate"
Leave a comment